“Please consider this communication as an SOS call from Liberia.”
“Please consider this communication as an SOS call from Liberia.”
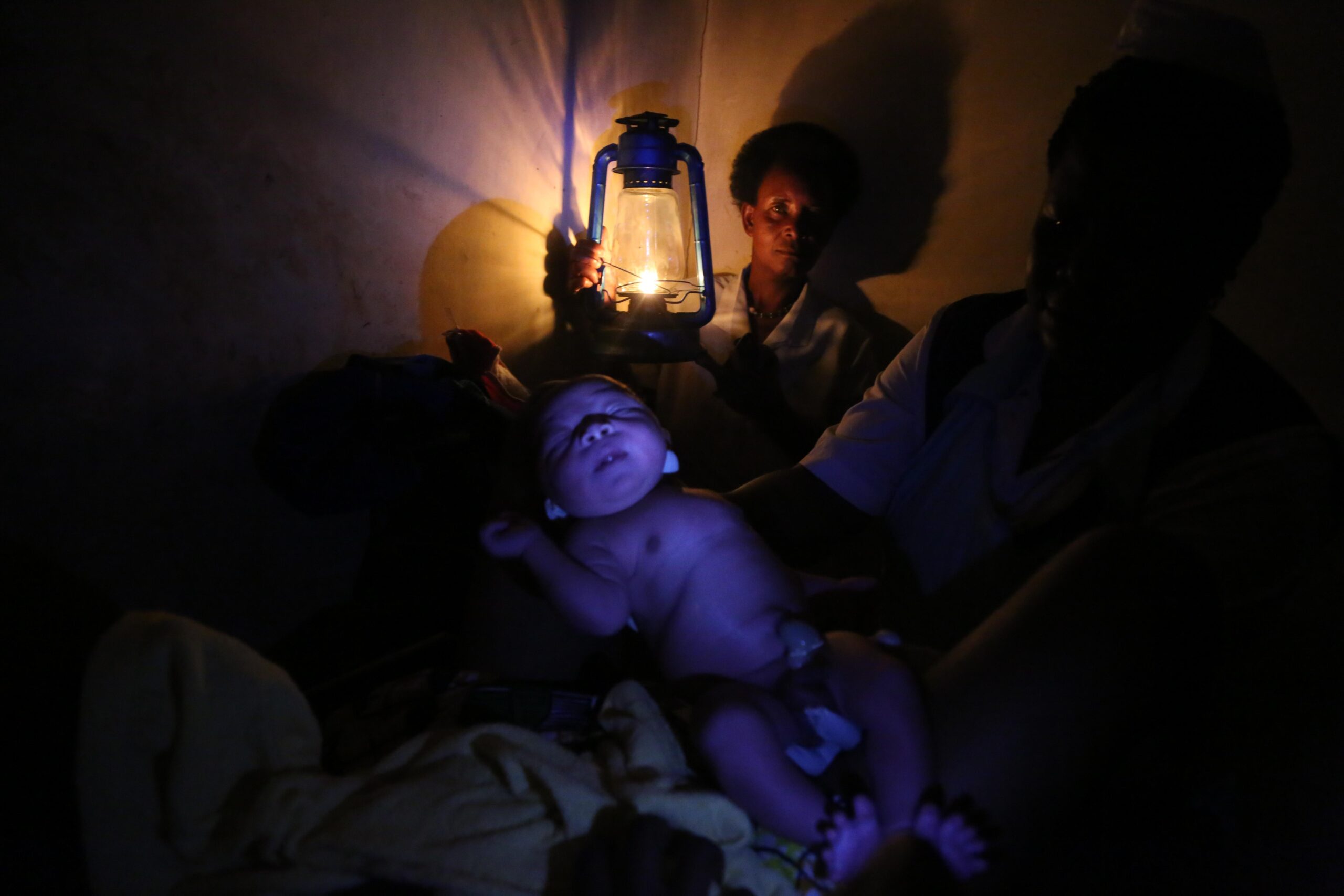
Bentoe Tehoungue, Director of Family Health at the Liberian Ministry of Health, sent out an email calling for help in facing the pandemic. But her primary request this week wasn’t for ventilators, PPE, or even oxygen to respond to the spread of the coronavirus, it was a call for light and electricity.
The COVID-19 pandemic is not only exposing glaring deficiencies in fragile health systems— Liberia has less than a handful of working ventilators in the whole country—it is threatening to erode hard-earned gains in maternal-child health care. Globally, more than 300,000 women die every year from complications of pregnancy and childbirth, predominantly in Africa and Southeast Asia. Most of these deaths could be prevented with prompt access to emergency obstetric care. High maternal mortality rates occur in regions marked by widespread poverty, limited education, scant antenatal care, and other factors leading to delays in identifying and treating pregnancy complications. For years, public health agencies have been steadily working to improve MCH indicators: building a network of community health workers, discouraging home deliveries, developing emergency transport schemes, boosting midwifery skills, and improving health care infrastructure. By providing light and essential power to health facilities, We Care Solar has become part of this equation. Solar Suitcases make it easier for health workers to provide quality services and thus increase the likelihood that women will deliver with skilled clinicians.
Policymakers and development organizations have hard decisions to make: how to focus on COVID-19 without dismantling many of these achievements.
“We have learned from the Ebola experience,” Bentoe states, recalling long-term consequences of another deadly virus. “We are trying to strengthen the normal services so we don’t have the adverse effects we had with Ebola.” During that epidemic, more women chose to deliver at home, fearing health centers as potential sites of disease. It is estimated that the indirect obstetric and newborn deaths from home deliveries in Sierra Leone, Liberia, and Guinea were as numerous as the direct deaths from Ebola itself.[1]
Ministries of Health in Liberia and other countries are working to avoid a replay of that scenario. While health officials try to build an arsenal of ventilators and oxygen concentrators for designated COVID-19 medical centers, they also continue to push for basic essential services in lower-level centers, including maternal and newborn care. Bentoe is part of the Liberian team working to mobilize protective gear for every health facility and set up triage stations and isolation rooms. To provide quality medical care, health workers need personal protective equipment, basic supplies, like thermometers, soap, and water, and brightly lit spaces to triage and isolate people with symptoms until they can be transported to higher-level facilities. As frightening as COVID-19 is for health workers in high-income countries, imagine the experience of health workers who are expected to provide frontline care in near-darkness.
If health workers are unprepared with protective gear and basic supplies, their personal fear is overwhelming and the consequences on health services can be disastrous. Liberia has already seen cases where health workers have turned away expectant mothers in labor– resulting in deliveries without skilled providers or equipment. “One mother gave birth in a home adjacent to the health center after she was turned away from the clinic,” Bentoe reports. “Another tried to walk home and gave birth in the community being assisted by an unskilled attendant as well.”
“COVID-19 has increased the need for lighting at ALL of our facilities,” Bentoe continues, “and added the burden for lighting critical areas in the health facilities, including the triage station, isolation areas among others. This SOS call is requesting We Care Solar and its donors/partners to consider providing Liberia with some Solar Suitcases to help us address this serious problem that has the potential to affect the women we are trying very hard to serve and protect.”
These concerns are not unique to Liberia and we are receiving similar requests from our partners in other countries. Dr. Charles Olaro, Director of Curative Services at the Ministry of Health in Uganda, has requested solar electricity for Isolation Centers and Primary Health Care facilities. “Definitely, electricity even without COVID-19 is one of the essentials you need for effective service delivery. But now with COVID-19 it is more essential in terms of infection prevention and control, you will even need electricity much more, both at the points of isolation but also at the points of quarantine.” While the country gears up to respond to anticipated increases in infection rates, he fears the impact on other health outcomes. “We don’t want to lose focus and have more deaths from causes other than COVID. You want to be sure that mothers will still be able to access services, they will be able to deliver. You need to deliver in terms of emergencies, surgical care, and any other services that are needed. So electricity is essential, with or without COVID.”
Dr. Olaro’s comments were echoed by Dr. Bernard Madzima at the Ministry of Health in Zimbabwe. “In Zimbabwe, we know the health system was already challenged before COVID-19 and this makes things worse. We have confirmed cases of COVID-19 and we have to be ready for the worst-case scenario. It has become even more important to have electricity now.”
Although the situation is challenging, COVID-19 also offers an opportunity. The global attention on public health care provides a spotlight on deficiencies in infrastructure that have plagued African health centers for decades: a lack of running water, inadequate supplies of standard equipment and unreliable electricity. With this spotlight comes an opportunity to accelerate efforts to achieve sustainable energy for all health care institutions.
At We Care Solar, we are increasing our efforts to equip health centers with reliable light and essential electricity. We are sourcing infrared thermometers powered with batteries that can be re-charged by the Solar Suitcase. We are offering our Solar Suitcases to support health workers in COVID-19 isolation centers converted from school rooms and community centers.
And we are accelerating efforts to support maternal health care workers, who remain a cornerstone of public health efforts. We are part of a global coalition that is calling for clean energy for health care, now and for future generations, with champions from SE4ALL, the World Bank, the United Nations, the WHO, and other institutions.
As Dr. Madzima reminds us, “For us, having light should be part of the protective equipment. At the health facilities that are going to be dealing with COVID-19, they should have adequate light for testing, for isolation, and for adequate treatment. We should take this as the opportunity to strengthen all the components of health system delivery, including infrastructure, including lighting.”
[1] https://academic.oup.com/heapol/article/32/suppl_3/iii32/4621472