On Monday, we flew to Jeremie, a coastal town to the West of Port-au-Prince that would have required a full-day of travel by car.
On Monday, we flew to Jeremie, a coastal town to the West of Port-au-Prince that would have required a full-day of travel by car.
The small plane took off, and soon we remembered that we were on a tropical island. Once in Jeremie, our eyes feasted on lush green plants and tropical flowers that cover the land. The topography is mountainous and beautiful, often affording a dramatic view of a river or ocean. The town of Jeremie itself is a wonderful flash to the past – well-kept wooden buildings boasting local businesses that have likely been going on for generations. We see chocolate beans drying on the porch, and taste mouth watering local foods.
Our host for this part of the excursion is Betty Gebrian, an energetic nurse who fell in love with this region more than 25 years ago, and now is Director of Public Health for the Haitian Health Foundation (HHF), an amazing community health program based in Jeremy . Almost without a pause, she took Brent and I on a narrated tour that ended up at a monthly health clinic, housed in a remote church situated in a breathtakingly beautiful location. HHF has created a stunning array of public health programs, recognizing that maternal health improvements must be placed in the context of community health.
The monthly health clinic is one example. The church I mentioned was bustling with people and activity when we arrived. The church office had been transformed into an obstetric clinic. HHF keeps careful records on every pregnant patient in the more than 100 villages they serve. A health worker checked in each woman, who then waited for a private appointment with the midwife and health workers. Each woman has her own health record, as well as a birth plan. While more than 90% of the population delivers at home, HHF encourages skilled care and an evacuation plan – a must for pregnant women who may face unanticipated complications during labor. The birth plan allows women to think through their myriad of choices. Will they deliver at home or in a hospital? How will they get from home to a hospital? Who will care for their children at home if they need to leave? What are the supplies they need for a home versus a hospital birth? The HHF program provides health education and has many novel ways of encouraging regular prenatal care (a generous layette for the baby given at the first post-partum visit) and teaching the danger signs of pregnancy (educational songs written by villagers themselves). Bette suggests to one VERY pregnant woman that she sing one of the songs, and soon a chorus of pregnant women were singing a bright tune that reviewed the major warning signs of late pregnancy – headaches, bleeding, swollen legs, etc. It was a clever strategy, one of many brilliant HHF programs that Bette described over the next few hours.
The main sanctuary hall of the church looked more like a health fair than a place of worship. The room had been divided into different stations: one was a pediatric health care station, complete with weight and measurement, another was a blood pressure station, another provided adult health care, while another was a pharmacy. HHF charges minimal fees for pediatric and adult care, which are inclusive of the costs of medication. So no one is penalized financially for needing additional care. Outside of the church was an outdoor dental clinic. Several volunteer dentists cared for a line of patients. There was a table for sterilizing instruments, another that displayed an array of shiny metal gear, gauze, and surgical gloves. Three dental chairs were placed on the grass, each with a panoramic view of the lush surroundings. Adult patients were getting dental care!
Even though a major focus of HHF is reducing maternal mortality, they recognize the importance of elevating the health of the whole family, and their programs reflect this. One program I especially appreciated was a program to postpone early pregnancy and promote healthy behaviors. HHF sponsors soccer teams for girls linked to health promotion programs! The girls learn about anatomy, reproduction, life skills (how to say “no” for example, and how to avoid risky situations) as well as soccer. While they initially wondered what level of community support they would encounter, the soccer games now draw 1000’s of local supporters! And HHF is tracking the girls over time. Even the prenatal records reveal which expectant moms had participated in soccer when she was younger.
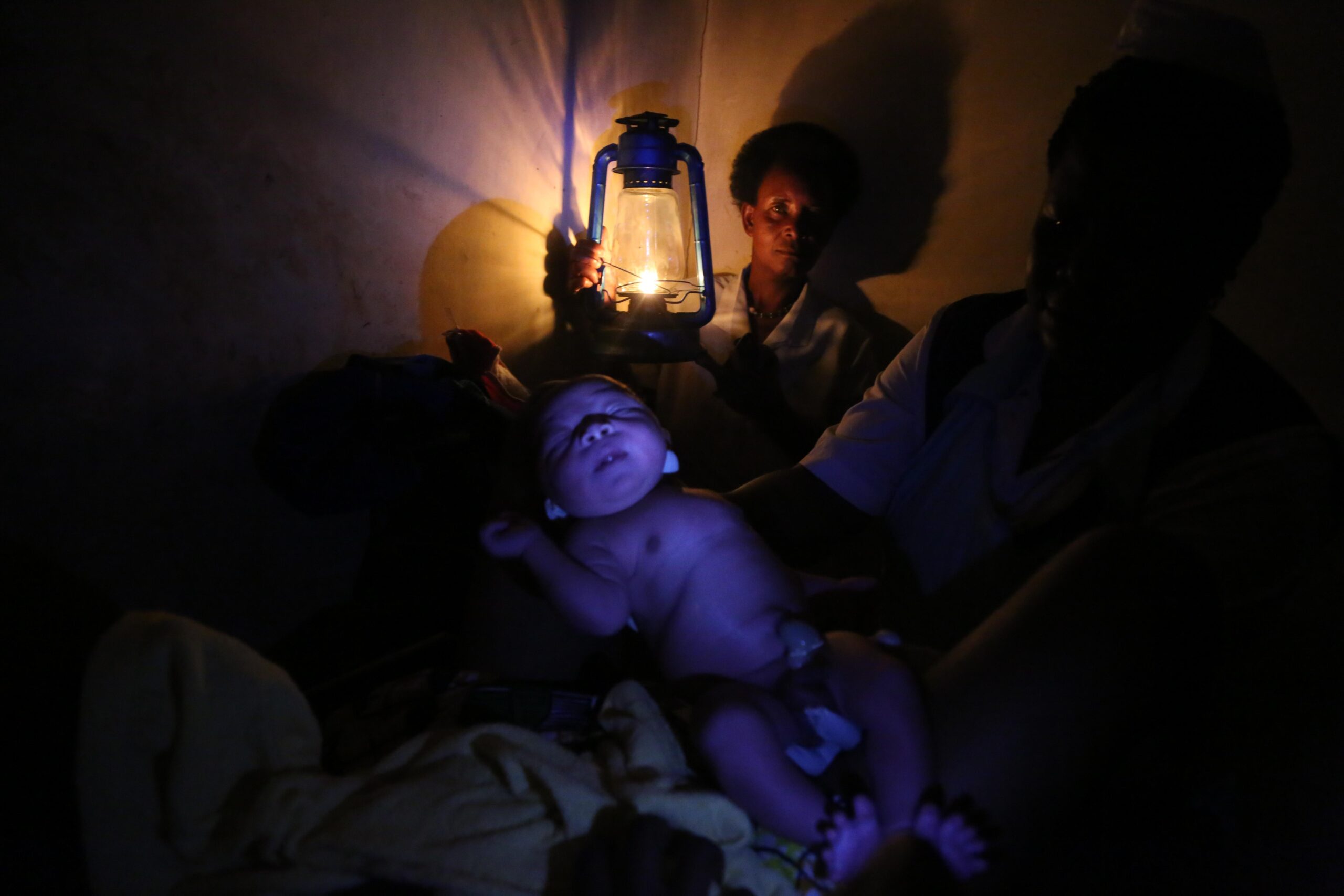
We made our way to the opposite side of the church, where a number of older men and women were lined up in chairs, after walking for hours to come here to meet us. These elders were actually the health attendants linked to HHF – they were the birth attendants for many of the villages in this area. It turns out that being a birth attendant is an acceptable role for men as well as women, and agism isn’t a problem. The average age of the birth attendants is sixty! I peered into the sparkling eyes of one of these health workers and asked his age (sixty-ten was the rough translation, or 70!) and how he became interested in birthing (“It came to me in a dream when I was young.”) The group had been assembled because WE CARE Solar had offered to provide headlamps and another solar suitcase to this area after Bette had written to me to let me know how useful the headlamps were for the health workers who practiced in a region with NO electric grid. “We could use hundreds,” she informed me, a statement which prompted our current “Mother’s Day Campaign.” I asked these noble workers to describe the realities of working without reliable light. “It’s windy,” I was told, “and the candles and lanterns blow out at night. We can’t see our patients.” I heard a description from one birth attendant of the challenges of assisting with a difficult birth without adequate light – about the stress and danger of working in these conditions. I also learned that the attendants care for children as well and have a successful program to treat pneumonia. One man lamented that he was unable to adequate evaluate a child for pneumonia at night. “We can’t watch their breathing pattern or see if they have retractions,” I was told, “so we can only evaluate them with our hands, placing our hand on their chest to feel their pattern of breathing, which we know we shouldn’t do.”
I was moved by their dedication and their experience, and marveled at how wonderful it was to utilize these experienced elders as accouchers (birth attendants). Bette invited me to address this group, and I told them a bit about my own experience as a doctor, my efforts to improve emergency obstetric care around the world, and how much I appreciated their efforts. I knew that HHF had developed a fantastic program to move high risk women to the “Center of Hope,” a building housing high-risk patients until delivery, and another program to evacuate and transport women to the hospital when complications were detected during labor. ““We are all one family,” I offered, “and the work you are doing is so very important. We are all trying to help save mothers and babies, and when you identify the women who need extra care or have complications, you are working as a team with the hospital workers to save lives.”
Brent and I handed out the headlamps we had carried from Berkeley, CA and demonstrated the solar suitcase that would recharge the batteries we had placed within each headlamp. The birth attendants were beaming as they each tried on their own headlamps.”We appreciate so much the work you are doing,” I added. “I know your work is very hard. But when you use these lights, remember that you have brothers and sisters in America who support what you are doing.” They told me how much this would help them in their work, and one asked if she could sing a song of thanks. I knew that for this small ceremony, HHF had only selected a fraction of the hundreds of health workers caring for women and their families, knowing that our supply of headlamps was very limited. I informed the health providers about our Mother’s Day Campaign, and that we hoped to send enough lights for all of the workers. “I hope that one day soon your mountains will be covered with lights,” I concluded.
Fresh coconuts were cut with a machete, and soon we were enjoying fresh coconut milk to celebrate. As Brent and I made our way back by car, I marveled at the miraculous chain of events over the last year that brought us to this moment. I marveled about HHF – a virtual model of “best practices” in community medicine – and the wonderful workers who are truly on the front lines of maternal health care. And it is truly a gift that we can play a small role in improving maternal health care in this region.